Think about your daily morning routine: rolling over in bed, reaching with your hand to turn on your bedside lamp, rising slowly to make breakfast, showering, dropping your bottle of shampoo, picking it up with your hand, brushing your teeth while holding the handle with all five fingers, and getting dressed, tying your shoes by wrapping the laces around your fingers to finish the double knot. Maybe you go to work and lift heavy objects or sit at a computer to organize files for your company, licking your fingertip every time you flip through a folder of papers.
Think about your daily morning routine: rolling over in bed, reaching with your hand to turn on your bedside lamp, rising slowly to make breakfast, showering, dropping your bottle of shampoo, picking it up with your hand, brushing your teeth while holding the handle with all five fingers, and getting dressed, tying your shoes by wrapping the laces around your fingers to finish the double knot. Maybe you go to work and lift heavy objects or sit at a computer to organize files for your company, licking your fingertip every time you flip through a folder of papers.
Now, imagine this routine with three fewer fingers on your dominant hand. There would be three fewer fingers to grasp your tooth brush or pull on your shirt. Should you have a desk job or one consisting of manual labor, your ability to efficiently do work diminishes.
Thirty-nine-year-old Eddie Chapman became someone who had to confront this imagined setback when he was in an accident at his job, losing his middle, ring, and little finger in a machinery malfunction. This accident made him one of the nearly two million living amputees in America. Not only did the amputation create physical difficulty in Eddie’s life as he could no longer complete the manual labor required at his job, it also caused mental barriers by creating a lack of self-esteem and confidence in his everyday actions. He could no longer accomplish the simple things he once could.
Eddie planned on receiving a myoelectric prosthetic, which uses small sensors implanted in the patient’s stump to transfer the natural electric signals from muscles to power the movement of the artificial limb. However, it has been noted by a variety of medical journals for decades that myoelectric prosthetics can be unreliable due to a concept called cross-talk.
During this cross-talk, the intricate muscular system of the hand forces these sensors to be placed close together, sometimes creating overlap or misinterpretation of signals. These faulty signals ultimately result in unwanted or incorrect prosthetic movement. In the case of trans metacarpal (partial hand) amputees, the muscles between the fingers meeting in the knuckle area were found to be causing the majority of this signal-error problem.
To combat this cross-talk of signals, doctors in Charlotte, North Carolina – Glenn Gaston and Bryan Loeffler – worked together with coworkers at OrthoCarolina and nearby HangerClinic prosthetic company to successfully develop a new surgery: the Starfish Procedure. This procedure helped Eddie along with six other partial hand amputees to regain their confidence and their lifestyles.
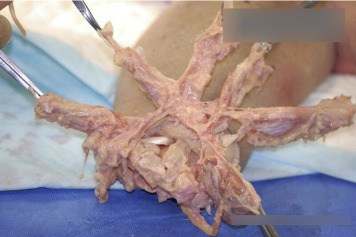
During this new and innovative surgery, the muscles with excess proximity in the hand (the ones causing the cross-talk) are dissected apart and placed in locations farther apart from each other. This results in greater likelihood of independent detection by the myoelectric sensors while maintaining nerve and blood supply at the same time. With the success in this surgery, the disruption and lack of accuracy in signal interpretation is drastically decreased. The name of the surgery, “Starfish Procedure,” comes from the appearance of the muscles mid-dissection resembling the body of a starfish, as shown in the image below, and the animal’s association with regeneration after losing limbs.
This surgery was completed seven times with no failure, showing promise for its future development. However, some experts doubt the predicted success of exploring the procedure with more proximal amputations because of the procedure’s high cost and the uncertainty of the prediction from lack of research. In 2016, there was a recorded 40% abandonment rate of myoelectric, showing a current issue with myoelectric rejection in these cases where amputation occurs further up on the limb.
The process of finding the surgery’s viability in these instances has already begun with researchers Bergmeister, Konstantin D, et al. conducting and reporting on a large animal study. His study explored the function of myoelectric prosthetics in four sheep and twenty-four rats with full limb amputations. Not only did the study conclude successful implantation and machine function of the electrodes in all animals involved in the study, it also showed the possibility of myoelectric function working better in more proximal amputations.
The muscles involved with myoelectric sensors in higher level amputees (most of/ full limb removal) are larger and more spread out than those associated with digit amputation in the hand, so there is less expected cross-talk between signals in the former. This large animal study shows that the Starfish Procedure may be different and less invasive, thus less expensive, while still achieving optimal control in prosthesis.
If given the proper resources to explore the surgery’s potential in more severe amputation cases, the Starfish Procedure could revolutionize the field of prosthetics. The reliability of the myoelectric product would be enhanced, and amputees would regain higher levels of functionality. They would get the small elements of their daily lifestyles back. They would be able to hold their toothbrush upright, tie a double knot, and pick up that slippery bottle of shampoo.
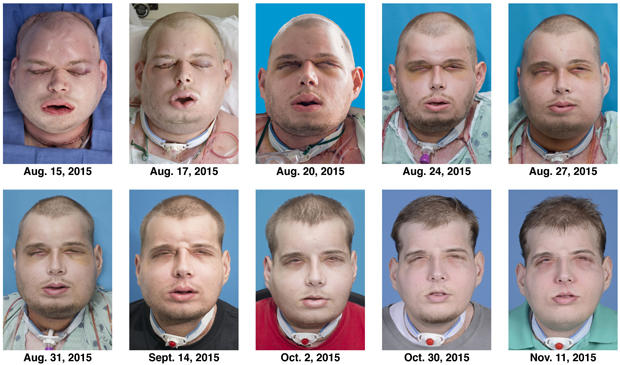
In an interview six months post-surgery, Eddie Chapman explained his increased sense of self-esteem following the procedure’s success. At two years post-op, Eddie can lift 20-pound dumbbells with his partially prosthetic hand, and he could not be happier. The Starfish Procedure’s success in improving the functionality of Eddie and the six other partial hand amputees shows that there is promise for further development of the procedure in more severe amputation cases.
With advanced exploration of this ground-breaking procedure’s potential, even more of the two million amputees in the nation can improve upon their prosthetic functionality as well.
By: K. Burgess
References:
“Amputee Hand Surgery: The Starfish Procedure.” OrthoCarolina, 23 Apr. 2018, www.orthocarolina.com/media/a-breakthrough-in-medical-care-the-starfish-procedure.
Bergmeister, Konstantin D, et al. “Prosthesis Control with an Implantable Multichannel Wireless Electromyography System for High-Level Amputees: A Large-Animal Study.” Plastic and Reconstructive Surgery, Vol. 137, Iss. 1: pp 153–162, U.S. National Library of Medicine, PubMed, Jan. 2016, https://journals.lww.com/plasreconsurg/fulltext/2016/01000/Prosthesis_Control_with_an_Implantable.30.aspx.
Chadwell, Alix, et al. “The Reality of Myoelectric Prostheses: Understanding What Makes These Devices Difficult for Some Users to Control.” Frontiers in Neurorobotics, Vol. 10, Iss. 7, Frontiers Media S.A., 22 Aug. 2016, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4992705/pdf/fnbot-10-00007.pdf.
Gaston, R. Glenn, et al. “A Novel Muscle Transfer for Independent Digital Control of a Myoelectric Prosthesis: The Starfish Procedure.” The Journal of Hand Surgery, Vol. 44, Iss. 2, pp 163.e1-163.e5, W.B. Saunders, February 2019, www.sciencedirect.com/science/article/pii/S0363502317314429.
Geethanjali, Purushothaman. “Myoelectric Control of Prosthetic Hands: State-of-the-Art Review.” Medical Devices (Auckland, N.Z.), Vol. 9, pp. 247-55, Dove Medical Press, 27 July 2016,
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4968852/.
Image Credits:
Image 1: Boyer, Massimo, “Sea Star Regenerating Arms,” https://plantandanimaladaptations.weebly.com/sea-star-5-arms.html
Image 2: Clinical Image from “A Novel Muscle Transfer for Independent Digital Control of a Myoelectric Prosthesis: The Starfish Procedure.,” https://www.sciencedirect.com/science/article/pii/S0363502317314429?via%3Dihub