“ah_designs” (2017). A person locked inside a pill bottle – prescription drug addiction concept stock illustration [Online image]. John Hopkins Medicine.
Rachel Lipari and her coworkers reported in 2017 that prescription drug misuse is the second most used illicit drug.
You are sitting in the operation chair ready to have your wisdom tooth removed. You are nervous, but you reassure yourself that it is a standard procedure that many people have done, and, usually, it is low stakes. You start counting down from one-hundred as you doze into oblivion.
The procedure is now over and you are dwindling back into consciousness. As the doctor is telling you the procedure was successful, you are prescribed 30mg daily of Oxycodone for two weeks without an explanation of what oxycodone even is. Once you are finished with the first bottle, you call your doctor and ask for a refill because your pain is still there. Your physician refills the prescription with no hesitation—and thirty days later you are now mentally and physiologically addicted to Oxycodone.
This scenario depicts how simple it is to become addicted to opioids, especially with the help of a provider’s prescription. According to physician, Martin Mackary and his coworkers, there were 240 million opioid prescriptions dispensed in 2015, nearly one prescription for every adult in the general population. In the 2000s, 75 percent of opioids users became addicted from a prescription pill.
Opioids are prescribed for moderate to severe acute illnesses, as well as chronic pain. Mackary argues that too many people are leaving the hospital with prescriptions they do not need. According to the Centers for Disease Control and Prevention, more than 165,000 died of prescription opioid overdoses between 1999 and 2014. Without doubt, an increased amount of prescriptions for opioids and improper or lack of education of risks, is enough for patients to fall victim to the opioid epidemic. An opioid prescription should be the last resort and other medications or non-pharmaceutical therapies can substitute.
In the late 1990s, pharmaceutical companies reassured the medical community that patients would not become addicted to opioid medications. According to the National Institute on Drug Abuse, opioid medications were prescribed at greater rates due to their reassurance that patients would not become dependent. However, since that time, researchers now understand that opioids are extremely addictive, and patients are now suffering from the repercussions.
Prescription opioids can be classified as oxycodone, hydrocodone, codeine, morphine, and fentanyl.
Opioids block pain receptors and trigger a release of dopamine which, create a euphoric feeling. With prolonged use of opioids, your body begins to function at a slower rate and when opioid use is stopped, users experience detrimental side effects.
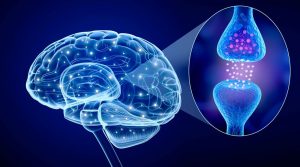
Addiction can go beyond mental factors for opioid users, as their body becomes dependent as well; therefore any opioid use can be dangerous. Opioids affect many parts of the body, including the hippocampus and hypothalamus in the brain. Abrupt stopping of opioid intake causes immense pain, even for everyday discomforts. The hippocampus, that is in control of emotions, goes into overdrive, causing feelings of anxiety. The hypothalamus, the body’s thermostat, goes haywire and the sweat glands perspire profusely regardless of the body’s internal temperature.
In addition, opioids affect the digestive system, causing constipation, therefore withdrawal symptoms may include vomiting and diarrhea, as the body begins to rid wastes.
Researchers are seeing a variety of misuses of opioids is seen in my ways. Medline Plus states that at times prescriptions are not always used by the sole person it was intended for, as some patients also share with their friends and family. Or, the patient takes more than was instructed.
But opioid misuse should not just fall on the patient. Physicians have a responsibility to prevent their patients from experiencing increased risks for addiction.
Patients with a past medical history of opioid misuse are at higher risks of relapse, yet they can obtain a prescription.
Seth Mnookin, a writer and ex-heroin addict, uses his personal narrative to describe his hospital trip after his appendix exploded. According to Seth, he was given Oxycodone without consultation, even after notifying his medical team his past history of hard drug use. He claims that his providers ignored his concerns and he began to experience withdrawal symptoms which slowed his healing process. The hospital Seth stayed in considers itself as one of the best in the country; however after confronting his surgeon, the surgeon shared the same frustration with the hospital as he did. The surgeon expressed:
“At the moment, we’re not getting a lot of guidance. And the addiction specialists are few and far between.”
What Seth Mnookin’s story highlights, is the failure of physicians and hospitals to provide proper counseling about the misuse of opioids. This failure could be the result of inefficient hospital regulations, and/or the lack of guidance provided to doctors for such medications. The CDC released new guidelines for practitioners to follow in 2016—however, these guidelines are voluntary. The CDC provides twelve recommendations for opioid regulation, but the American Medical Association remains concerned that the science behind some of the recommendations are too vague, conflict with state laws, and, as a result, they believe patients may suffer the inaccessibility to non-pharmacologic treatments.
Nevertheless, stated by researcher, Thomas Sullivan, the recommendations provided by the CDC such as: discussing risks and benefits, using the lowest effective dose, establishing goals for pain and function, and drug testing are helpful because they provide a backup for providers. Also, CDC recommendations allows providers to educate their patients about the dangers of opioids.
Despite the CDC providing regulations, Rachel Lipari and her coworkers reported in 2017 that prescription drug misuse remains the second most used illicit drug. It is clear that more work needs to be done and these guidelines need to be actively regulated and enforced. The CDC must continue to address relevant issues that raise a concern for both physicians and patients.
Physician, Dr. Harris underscores the American Medical Association statements by stating that:
“If these guidelines help reduce the deaths resulting from opioids, they will prove to be valuable. If they produce unintended consequences, we will need to mitigate them. They are not the final word. More needs to be done, and we plan to continue working at the state and federal level to engage policy makers to take steps that will help end this epidemic.”
The CDC’s 2016 regulations are a stepping-stone that need improvement to reduce the number of patients unnecessarily being prescribed opioid medications, and thus the number of people becoming addicted. The medical community must continue to seek ways to improve education to prevent over-prescriptions of opioids to their patients.
By: C.Frazier
References
Compton, W. M., Jones, C. M., & Baldwin, G. T. (2016). Relationship between nonmedical prescription-opioid use and heroin use (D. L. Longo, Ed.). New England Journal of Medicine, 374(2), 154-163. doi:10.1056/nejmra1508490
Hogan, A. (2018, November 17). How opioid withdrawal forces body to come undone. Retrieved February 7, 2020, from https://www.statnews.com/2016/05/25/opioid-addiction-withdrawal-survival/
Lipari, R.N., Williams, M. and Van Horn, S.L. Why do adults misuse prescription drugs? The CBHSQ Report: July 27, 2017.Center for Behavioral Health Statistics and Quality, Substance Abuse and Mental Health Services Administration, Rockville, MD. Retrieved February 8, 2020, https://www.samhsa.gov/data/sites/default/files/report_3210/ShortReport-3210.html
Makary, M. A., Overton, H. N., & Wang, P. (2017). Overprescribing is major contributor to opioid crisis. BMJ (Online), 359, [j4792]. https://doi.org/10.1136/bmj.j4792
Mnookin, S. (2016, August 10). I’m an ex-addict. Why was it easy to get prescription opioids? Stat News. Retrieved February 8, 2020, from https://www.statnews.com/2016/06/09/opioid-prescriptions-addiction/
National Institute on Drug Abuse. (2019, January 22). Opioid Overdose Crisis. Retrieved from https://www.drugabuse.gov/drugs-abuse/opioids/opioid-overdose-crisis
Opioid Prescribing. (2016, March 16). Centers for Disease Control and Prevention. Retrieved February 8, 2020, from https://www.cdc.gov/features/opiod-prescribing-guide/index.html
Safe opioid use. (2019, October 18). Medline Plus. Retrieved February 8, 2020, from https://medlineplus.gov/safeopioiduse.html
Sullivan, T. (2018, May 5). CDC Releases Guidelines for Prescribing Opioids. Policy and Medicine. Retrieved February 9, 2020, from https://www.policymed.com/2016/03/cdc-releases-guidelines-for-prescribing-opioids.html
What physicians are saying about the new CDC Opioid guidelines. (2016, March 16). American Medical Association. Retrieved February 9, 2020, from https://www.ama-assn.org/delivering-care/opioids/what-physicians-are-saying-about-new-cdc-opioid-guidelines
Image Credits:
Image 1: “ah_designs” (2017). A person locked inside a pill bottle – prescription drug addiction concept stock illustration [Online image]. John Hopkins Medicine. https://www.hopkinsmedicine.org/opioids/science-of-addiction.html
Image 2: “alexmit.” Human brain and Active receptor [Online image]. Newport Academy. https://www.newportacademy.com/resources/mental-health/this-is-what-happens-to-your-brain-when-youre-addicted-to-opioids/